Initial outcomes at a small community Geri ED
A grass-roots movement for improved geriatric ED care
About Aurora Sheboygan Memorial Medical Centre
A small, community Geri ED in Sheboygan, Wisconsin
- 23,000 ED visits per year all ages
- 5,300 ED visits per year for those over 65
- Not a research hospital
- Non-academic status
- Not-for-profit institution
Needs Goals and Motivations
What drove your ED to work to improve care for older adults?
The Geri ED program at Aurora Sheboygan Memorial Medical Centre started in 2014 at the grass-roots level where a team of ED RNs & MDs came together to address the vulnerabilities of older adults who present in the ED but are discharged back to the community.
Why did you engage GEDC to help in your efforts?
The GEDC provided our team with a structured approach to evidence-based quality improvement, demonstrated innovative program examples, and motivated the team at our GED Bootcamp. The Bootcamp event motivated and empowered our small team with a sense of mission. The GEDC’s practical and hands-on approach provided the tools and skills for the team to improve care despite no additional resources.
Challenges and Drivers
What challenges did you face in implementing your quality improvement initiative?
The ED is a very unique environment with many competing priorities. The rationale for doing such a project was relatively straight forward because individuals became health care professional to help people. The biggest challenge was devising an interprofessional workflow that didn’t impact LOS and productivity.
Solutions
What were some solutions to the challenges you faced?
As we developed our protocols and interprofessional workflows we had difficulty knowing if we were achieving our process measures, much less our patient outcomes. We took a systematic approach to building the protocols in the EHR that supported the workflow and reporting. Then we standardized process measures and summary reports to provide regular feedback to each discipline and identify priority areas to improve. With this infrastructure we were able to support a process of continuous incremental improvement.
How was GEDC helpful in addressing these challenges?
The GEDC community has a broad range of expertise, whether it was clinical topics such as falls and delirium, or quality improvement, measurement, and evaluation. Our team was able to draw from this expertise per our specific needs during our journey.
Outcomes
What improvements have you seen in the ED since completing your GEDC training?
We have benefited from many changes over years, both quantifiable and qualifiable. The most significant is a change in culture and a sense of empowerment to positively improve care delivery.
Our nursing team has taken ownership of the process. They drive continuous improvement utilizing process measures and identifying new priorities. Quantifiable change is demonstrated with consistent screening/assessment rates, >30% reduction in 30day ED revisits, development & implementation of new clinical protocols, community partnerships (EMS, Dept of Aging), and achieving GED accreditation.
What process outcome measures are you continuing to evaluate?
We report ISAR (Identification of Seniors at Risk) screening rates, Timed Up and Go screening rates, patient mobility documentation, and associated service-to orders (PCP, out patient PT, Palliative, Homecare) monthly. Additionally, we are taking deep dives into patient outcomes, patterns of ED utilization, and cost effectiveness to develop return-on-investment outcomes.
Future Goals for Our ED
As we develop and implement more clinical protocols, we continuous refine with our data reporting, which will culminate in a Geri ED dashboard. Our goal is to achieve Level 2 GED Accreditation in 2020.
Below you can find an image of the fall protocol we use in our emergency department to evaluate older patients for safe mobility.
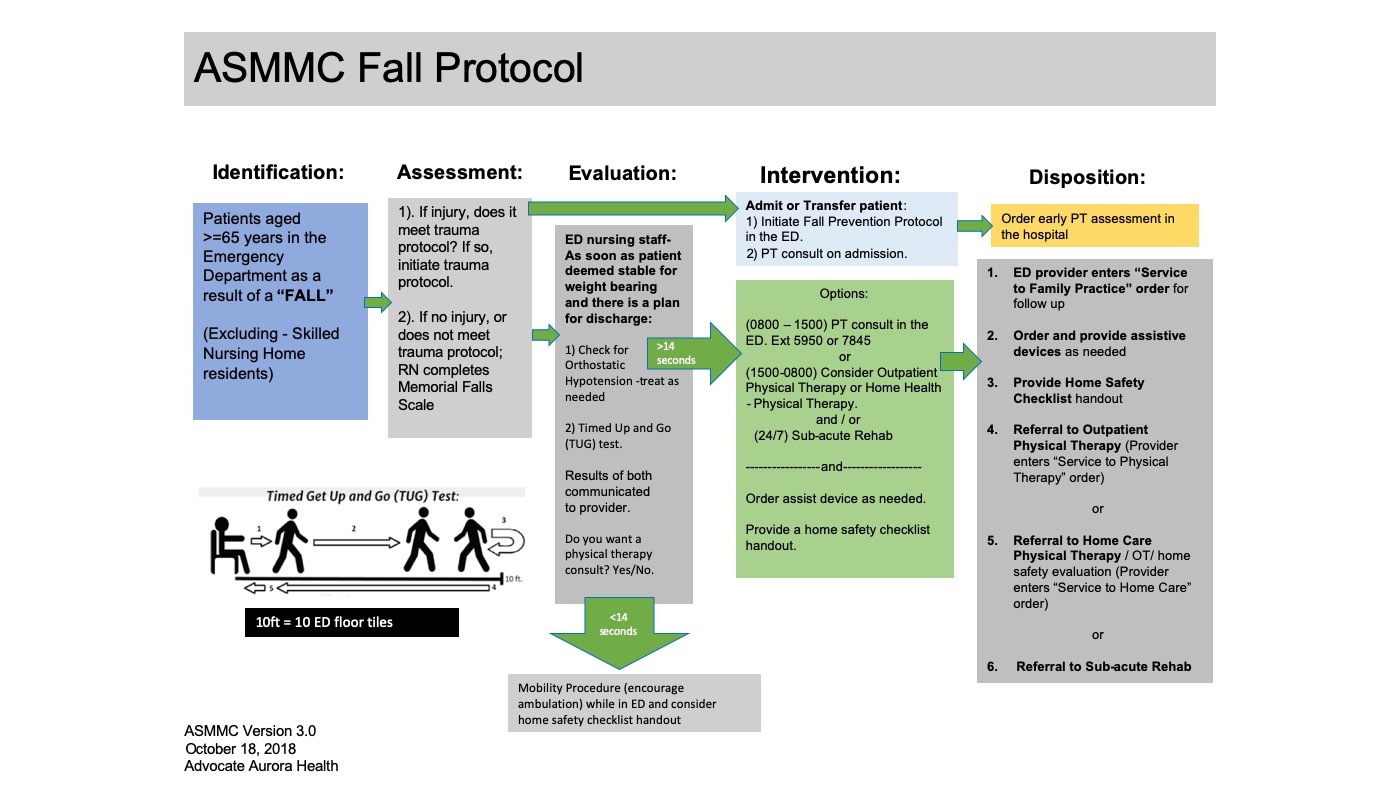 This is the Fall Protocol used by the Aurora Sheboygan Memorial Medical Centre Emergency Department.
This is the Fall Protocol used by the Aurora Sheboygan Memorial Medical Centre Emergency Department.