Boarding and Overcrowding of Emergency Departments: Implications for Older Patients
GED Newsletter, February 2019
GED Newsletter, February 2019Introduction
Boarding of patients in the Emergency Department means having those who are admitted to the hospital stay in the department for more than 4 hours after their admission. Further, “overcrowding” refers to the need to attend to more patients than for what the system and space was designed.
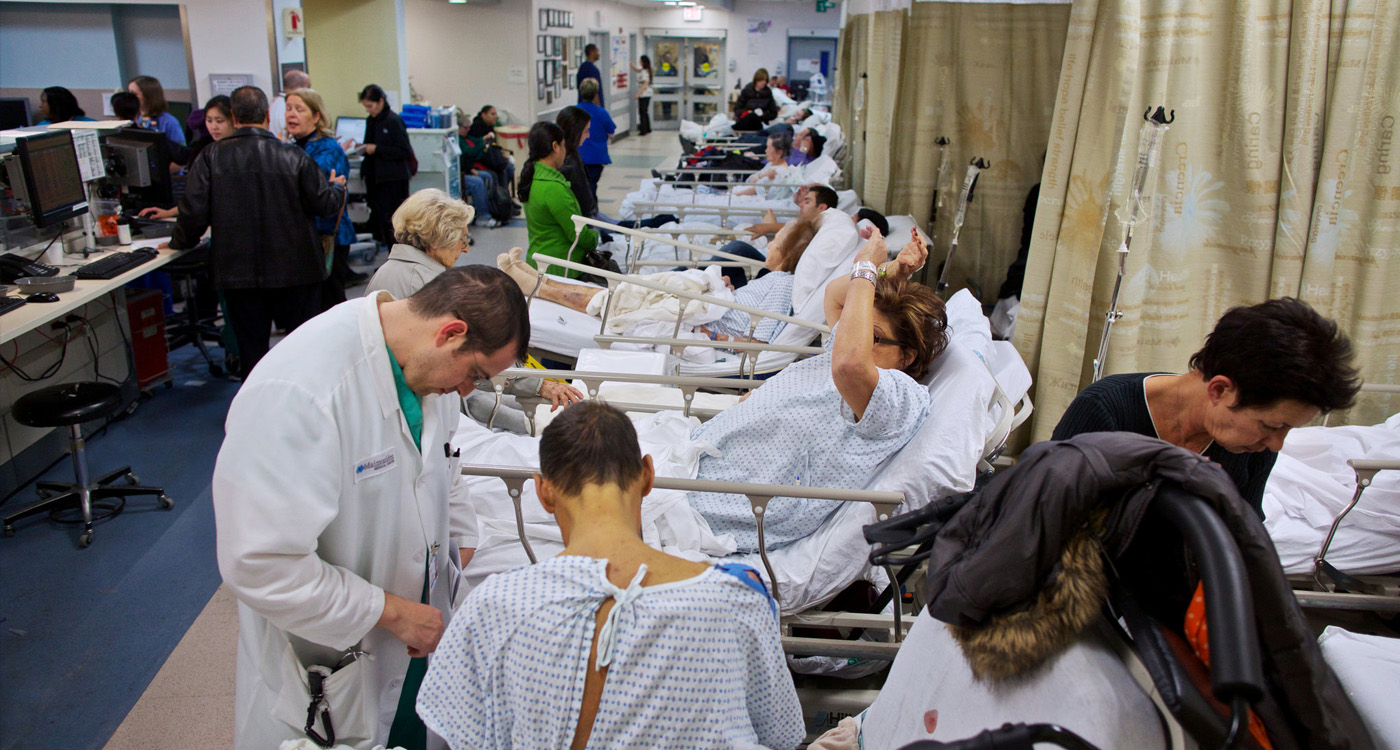 Overcrowding can be stressful for patients and family caregivers, as well as for those providing care.
Overcrowding can be stressful for patients and family caregivers, as well as for those providing care.
Some patients in very busy ED’s may have to stay hours to days, creating a setting where lots of folks are waiting in the midst of others who are critically ill or injured. Boarding and overcrowding may create a setting that is stressful for the patients and family caregivers as well as for those providing the care.
The underlying causes may include:
- outbreaks of influenza or respiratory illness
- policies to avoid the diversion of ambulances
- suboptimal scheduling of patients admitted for surgery
- throughput of hospital patients who actually could be transitioned to post-acute care, and poor access to post-acute services.
About ten percent of all patients admitted are boarded prior to receiving hospital care. Older adults make up 30-50% of boarded patients. Health outcomes of boarded patients have been described in the medical literature: one study described an increase in mortality, while another study noted no association with unanticipated death within the first 24 hours of care.
Key Points
When older adults are boarded in the Emergency Department several strategies are required:
- Develop a “safety and comfort” protocol for boarding older adults. This will include:
- hospital bed or recliner
- appropriate temperature
- quiet appropriately illuminated room
- easy access to food/drink
- distracting or preferred activities
- removal of “NPO status” as soon as possible
- frequent staff rounding
- Provide regular access to appropriate toileting facilities during the stay. Avoid placing a urinary catheter for convenience.
- Continue indicated outpatient management of chronic conditions such as diabetes, COPD, CHF, and Parkinson’s disease. This includes early medication reconciliation.
- Decrease risk of deconditioning by encouraging mobility and getting out of bed.
- Employ a delirium mitigation protocol for those older adults at increased risk, such as those with underlying dementia. This will include:
- frequent orientation
- maximal caregiver presence
- frequent toileting, nutrition and mobility
- trained employed or volunteer companions
- clear day/night distinction
- sensory devices, such as hearing amplification or reading glasses, as needed.
- Anticipate and prevent problems of dignity. Provide privacy during interactions as best as possible.
- Emphasize caregiver comfort and communication by frequent updates, nutrition, adequate seating, Wi-Fi, and parking assistance. Make efforts to ensure consistency of nursing care to better monitor the older adults for changes in condition and support patient and family.
- Review the systems based flow of patients with hospital leadership to improve the flow of patients. Look at patterns and practices to better address the needs of patients. Obtain Case Management and PT/OT evaluations onboarding patients who will need post-acute services.
- Work with the admitting services to clearly delineate responsibility for admitted patients boarding in the ED, including a protocol regarding rounding and orders for boarding patients.
- Develop a protocol to frequently review admission status for boarding patients to address:
- de-intensification (is the ICU or telemetry still appropriate?)
- admission versus observation status
- and need for continued admission.
References
Carpenter CR, Platts-Mills TF. Evolving pre-hospital emergency department and “inpatient” management models for geriatrics emergencies. Clin Geriatr Med 29: (2013) 31-47.

